Read our 2024 annual report

Knowledge Hub
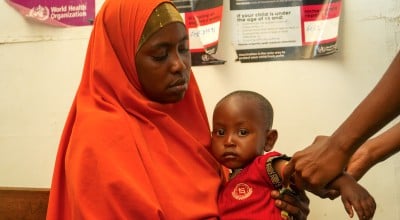
Inside nutrition clinics around Mogadishu, these healthcare workers do whatever it takes to save Somalia's most vulnerable.
More than 3.5 million people in Somalia have been internally displaced by a combination of conflict, drought, and flooding. Many of them end up in internally-displaced persons (IDP) camps on the outskirts of Mogadishu.
These sprawling settlements of makeshift shelters usually offer the bare-minimum for living conditions – even more so since funding cuts in overseas assistance. Families who land here struggle to meet basic needs.
As a result, roughly 1.84 million Somali children under the age of five are expected to face acute malnutrition in 2026. Tens of thousands are treated at one of several clinics around Mogadishu, including the Siinka Dheer and Wadajir Health Centres and the larger Banadir Hospital, all supported by Concern.


Wadajir Health Centre
“This programme is essential to the community,” says Dr. Zam Zam Ahmed, who specialises in maternal and child health at Wadajir – a 20-minute drive from downtown Mogadishu. It’s one of the biggest community health facilities in the area.
On a normal day, Dr. Ahmed adds, she and her colleagues diagnose at least 10 cases of severe acute malnutrition. Those children are admitted into Wadajir’s nutrition programme and provided with ready-to-use therapeutic food, a fortified peanut paste. The clinic also provides counselling on maternal and infant nutrition for mothers.
Additionally, Dr. Ahmed and her colleagues usually see at least 50 children for other medical issues, and deliver at least three babies each day.

Siinka Dheer
About 10 kilometers northwest of Wadajir is the Siinka Dheer clinic. Despite being further afield, Siinka Dheer sits at a critical point in Banadir, just across the border from the Lower Shabelle district, known as the Afgooye Corridor.
In 2010, the United Nations High Commissioner for Refugees described Afgooye as “the capital of Somalia’s displaced.” While Somalia’s internally displaced have become more spread out across the Mogadishu metro area, Afgooye still has a large IDP community and remains a critical access point for humanitarian aid and convoys.

“A normal day in Siinka Dheer is busy and challenging... There are a lot of people needing different kinds of assistance,” says Muqtar Deerow Luqman, Siinka Dheer’s Senior Supervisor.
In the mornings, Concern’s community healthcare workers visit the IDP camps in the area. They screen mothers and children for malnutrition and ensure that camp residents know what services are available to them.


“He took that risk so that his daughter could survive”
The services provided are free of charge, as families often risk everything to get to these camps. “During their journey here, [families] face different obstacles,” says Bihi Omar Wehlie, a Health and Nutrition Programme Officer for Concern Somalia.
“Some of the roads are affected by floods. Some of the roads are not accessible due to inter-clan conflict. Some people are from areas where people are not allowed to leave during the daytime. We have seen a lot of people who escaped during the night.”

Wehlie recalls one father, Raheem*, whose three-year-old daughter Faduma* became ill in their village in Somalia’s Lower Shabelle region, 75 kilometres away from Mogadishu. Faduma’s condition lasted for three weeks and didn’t improve, and so he decided to take his chances getting her to Mogadishu, setting out on foot at 3am and travelling through a forest full of wild animals.
“He had nothing, no weapon or tool to protect them,” Wehlie says. “He took that risk so that his daughter could survive.” Eventually, Raheem and Faduma were able to get a ride, landing in Afgooye. Friends and family told them to go to Banadir Hospital.


Banadir Hospital
Unlike Siinka Dheer and Wadajir, which function as community clinics, Banadir is a national hospital, and the largest in Somalia. With more resources and facilities, Banadir’s stabilisation centre is where children requiring inpatient treatment are often referred.
“The stabilisation centre is one of the busiest units in the hospital,” says Dr. Muhammad Dek Jama, who supervises the centre. When we spoke with Dr. Jama in early 2025, he reported that they had admitted over 500 patients in just three months.
Despite this level of need, Concern (with funding from Elsevier and UNICEF) is the only NGO supporting Banadir’s stabilisation centre, providing medical supplies, training, staff salaries, and other costs of operation. This support, as Bihi Omar Wehlie notes, is critical.

Back from the brink
Raheem and his daughter reached Banadir Hospital on Christmas Eve 2024. Faduma had acute diarrhoea and gastroenteritis and acute malnutrition. She weighed 4.4 kilograms, a normal weight for an infant of two or three months. Faduma, however, was three years old.
“Her condition was monitored every 30 minutes,” says Wehlie. “She received a blood transfusion. Her breathing was shallow, so she was administered oxygen therapy.”
For seven days, Faduma remained in critical condition. But in the early days of 2025, her condition began to improve. Banadir staff removed her feeding tube and catheter. She began her own course of therapeutic food, and her weight went from 4.4 kg to nearly 9kg.
“Before, she had a face like an old man. The muscles and tissues had wasted, but now she is improving,” Wehlie adds. Likewise, Raheem went from feeling hopeless to hopeful.

Continuing care
The day a patient is discharged is often a happy one, especially for parents like Raheem. However, it’s not the end of the involvement for healthcare workers at Banadir.
“On the day of discharge, we find out if there is an outpatient treatment centre where they live,” Wehlie explains. “If there is, we refer the child to that centre.” Many Banadir patients end up receiving follow-up care at one of 11 outpatient centres supported by Concern in Mogadishu, including Siinka Dheer and Wadajir.
This is a critical part of the process, Wehlie says, as children without access to an outpatient clinic are more likely to relapse, in some cases as quickly as a few days after being sent home. Fortunately, Raheem’s family in Mogadishu lived close enough to a centre for Faduma to receive ongoing checkups.


Getting ahead of the curve
The big challenge that clinics and hospitals face now, as Banadir Hospital’s Dr. Jama notes, is getting ahead of the curve when it comes to seasonal or situational “surges” in caseloads for malnutrition and other child illnesses.
“The staff couldn’t monitor the caseloads and couldn’t know which months the facility would go on ‘alert’ or into emergency mode,” he says. “Sometimes, in the middle of an operation, we would run out of supplies.”
Part of Concern’s support for Banadir is working with the staff on implementing the Surge Approach, a system that grew out of Concern’s standard-setting programme, Community Management of Acute Malnutrition. Rather than reacting to cases of malnutrition (and now other common illnesses), Surge takes a proactive approach, using weather and other available data to predict and plan around spikes in cases.

Facilities including Banadir have received Surge training as part of Concern’s Caafimaad Plus programme, which reached over 110,000 people in 2025. The approach has been such a success that Somalia’s Ministry of Health incorporated it into its national nutrition guidelines, with Concern leading the learning and pilot phase at the national level.
“We can predict which months the caseload will increase, and we know the probable causes of increases,” says Dr. Jama, with a sense of relief.
Why they stay
For a healthcare system that has been pushed to the brink, every tool like Surge goes a long way towards helping the helpers – ensuring that healthcare professionals avoid burnout and are able to keep treating the patients in their care.
But this isn’t the only thing that keeps these clinic and hospital staff showing up day after day. Dr. Ahmed, who has worked with Concern for seven years and was the first person in her family to become a doctor, recalls the brutal impacts of Somalia’s 2017 drought. At the time, she and some colleagues from the Somali Doctors’ Association began treating patients at some of the IDP camps.

“We saw a lot of people coming, suffering from the impact of conflict and drought,” she says. “That encouraged me to stay in Somalia and help people in need.” Three of her siblings have also followed her example, each graduating from medical school with different specialisations. “We’re a family of doctors,” she smiles.
“Why do I stay in Somalia? Because I know that I am Somali,” adds Dr. Jama, whose cousin supported him through medical school when his parents were unable to. He is now supporting his family. “I thought it is better to stay and support my family with the little I could have here.”
There are also the job benefits that can’t be quantified. For Siinka Dheer supervisor Muqtar Deerow Luqman, the best part of his job is seeing mothers and children get the help they need. “Watching their progress and seeing them regain their health is the most rewarding experience for me.”
Help us reach more people with lifesaving care