
Read our 2024 annual report

Knowledge Hub
It’s eerily quiet as Dr Hafsa Mohamed does her morning rounds at the stabilisation centre at Mogadishu’s Banadir Hospital — Somalia’s largest paediatric stabilisation centre for some of the sickest children currently enduring the region’s worst drought in 40 years.
Although the centre — which is supported by Concern and UNICEF — is full to capacity with all 75 beds occupied, there is scarcely a sound from the children lying in the beds during our visit. There’s no crying or whimpering from the toddlers sharing the ward while the doctor talks to their mothers.
Instead they are lifeless and limp in their beds, some with feeding tubes and hydration tubes taped to the sides of their heads, others caked with cream and hands covered in cardboard mittens.
Two-year-old Aaden* remains limp in his mother’s arms for the 10 minutes she takes her to tell his story. He was admitted a few days ago, severely acutely malnourished and weighing just 5.4kgs (12lbs). He was in shock from days of dehydration and vomiting. He was anaemic and needed a blood transfusion, Dr Mohamed notes.

Aaden is the youngest of eight children. The family live in one the many sprawling camps for displaced people which have sprung up around the Somali capital in recent years. They fled over 100km from Awdheegle district in the Lower Shabelle district, as a result of the drought and conflict.
Life in the displacement camps is difficult. “I wash clothes for families and my husband pulls a rickshaw to buy food, but we have nothing else. The other children are hungry. But we trust Allah and pray that things will get better,” his mother said.
The combination of the drought and conflict has driven many people to make the decision to move. Over 417,000 people have arrived in Mogadishu since January 2022, according to the UNCHR. In total, over one million Somalis have had to leave their homes as a result of the two-year drought.
We are very stressed. We are seeing a lot of severe cases.
Sagal* travelled 150km to Mogadishu with her husband and five children. They were farmers but the river they used to irrigate their land dried up. Their 15 cows have died.
She says she has never seen a drought like it and she lived through the 2011 and 2017 droughts. “The 2011 drought affected part of the region, but this drought has affected the whole region,” she said.
Sagal is at the stabilisation centre with her son, Taifa*. He had measles and developed complications, with diarrhoea and oedema following. The family took the decision to move for help.
Among the families gathered at the hospital are those who have lost children during the drought. Surad* has already buried two of her six children during the drought. “They died from the lack of food,” she explained.
Surad is at the clinic with her son, Cumar* (seven months). One of the nurses measures his middle upper arm circumference with the tape confirming that he is severely acutely malnourished – or in layman’s terms, he is experiencing life-threatening levels of hunger.

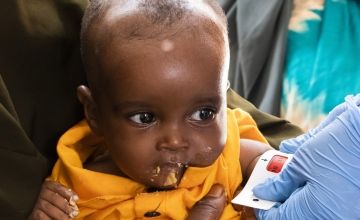
The family left their village in the Lower Shebelle region because of fighting and the drought. She has ambitious plans for her sick son. “My wish for him for the future is that he becomes a teacher or well-educated person,” she said.
For Dr Mohamed and her team, the work never ends. So far this year and up to the middle of December, they had treated 2,585 sick children aged under five. The 75 bed unit is almost continuously full and sometimes they have to turn sick children away. A 40 bed extension is currently under construction and is due to open early in 2023.
“We are very stressed,” she said. “We are seeing a lot of severe cases.” The sickest children who cannot be treated in community clinics are referred here. In addition to being malnourished, many have other complications such as whooping cough, measles or diarrhoea. Their immune systems are extremely weak and the combination of conditions is life-threatening.
But 95% of children treated at the clinic this year have survived. Just 172 patients have died so far in 2022.
Some of the mothers who arrive with sick children tell stories of losing children along the way. They often travel hundreds of kilometres from near the borders of Kenya and Ethiopia to get treatment, Dr Mohamed noted.


Yet they are the lucky ones. In addition to those who die on the road, others are too ill to be saved by the time they reach Mogadishu.
Not all children require hospitalisation, although they are malnourished. The Concern-supported Wadajir health and nutrition clinic a few kilometres away treats up to 140 mothers and children a day, rising to 160 patients some days.
Among those being treated the day I visited was Fowsio* whose tiny eight-month-old daughter Bilan* was being seen by the nutrition team. She was just 5.6 kgs (12lbs) when she arrived and was diagnosed as having life threatening levels of malnutrition.
Bilan is reacting well to the nutritional food supplements she is receiving. “She is getting heavy and happy,” her mother said. Bilan is one of nine children, all aged under nine years old. Three of them have been sick and Fowsio admits to struggling to feed them. “We have to accept what Allah gives us,” she said.
*Names have been changed.





